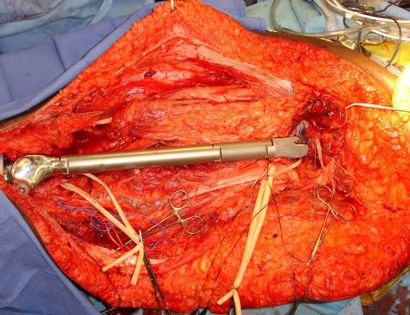
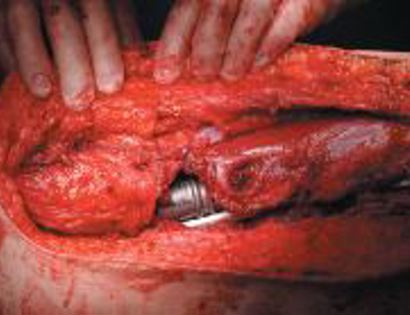
What is a Total Femur Prosthetic Replacement?
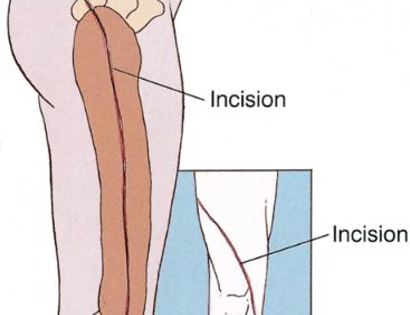
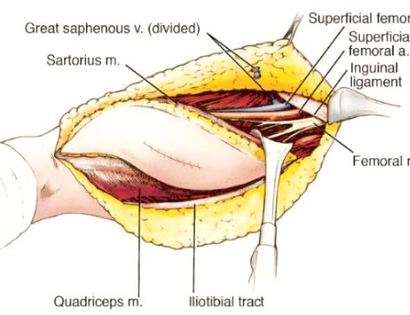
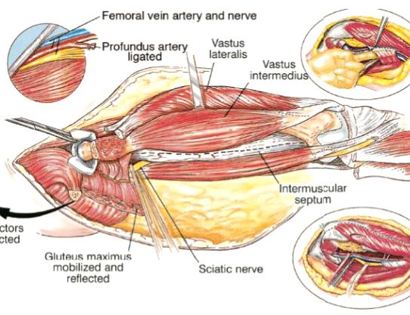
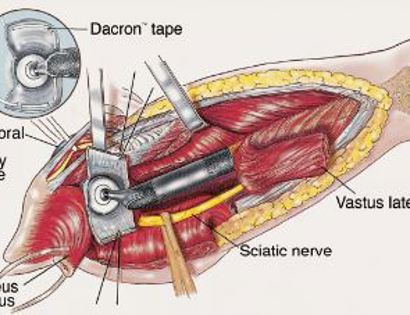
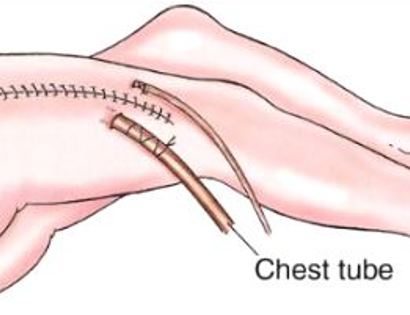
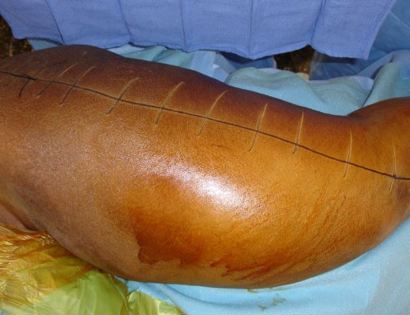
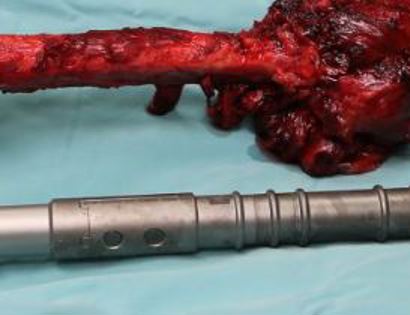
The femur is the long bone of your thigh and is important for proper function of the hip and knee joints. The entire femur is a relatively common site for primary sarcomas and metastatic disease. Some of these tumors include osteosarcoma, chondrosarcoma, and Ewing’s sarcoma. The common muscles of your femur (thigh bone) include your hamstrings and quadriceps. A total femur prosthetic replacement involves a radical resection of the femur containing the sarcoma and replacing the bone with a prosthesis. A total femur prosthetic replacement is considered a limb-sparing surgery. Limb-sparing surgery can be performed for approximately 95% of tumors arising from the upper femur. Adjuvant (additional) therapies, such as chemotherapy and/or radiation, may be used in conjunction with this procedure as treatment for various bone sarcomas. In some instances, the extremity cannot be saved and an amputation is performed.
Contraindications for saving the limb may include neurovascular invasion, infection, pathological fracture, invasion of the pelvis, extensive disease, contamination from a poorly performed biopsy, recurrent disease.