Soft Tissue Sarcoma Resections
It is a procedure that involves removing a tumor (malignant or benign) of the soft tissues (muscle or fat) while preserving the surrounding healthy bone and soft tissues.
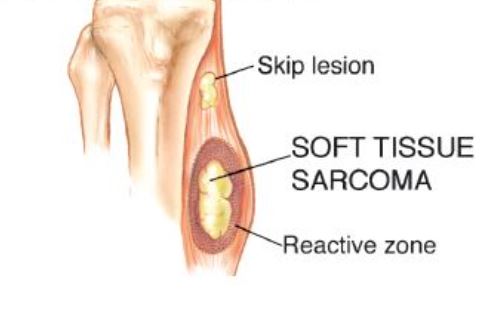
It is a procedure that involves removing a tumor (malignant or benign) of the soft tissues (muscle or fat) while preserving the surrounding healthy bone and soft tissues.

Soft-tissue tumors or soft-tissue sarcomas most commonly arise from the deep muscles of the extremity (limb). The thigh is the most common site, however, a soft-tissue sarcoma can really arise from any part of the body including any extremity including buttock, back, shoulder, arm, forearm, hands, feet, or calves. They generally present as a painless mass that has increased in size over some time period. They may cause pain in some cases. Occasionally, a patient may give a history of a previous trauma or injury to the area that really has nothing to do with development of the soft-tissue tumor. MRI imaging is used to view the soft-tissue tumor, but a biopsy may be warranted if there is uncertainty or suspicion of malignancy (cancerous) in order to obtain a definitive diagnosis. Some of the most common benign soft tissue tumors include lipomas, schwannomas, and hemangioma. Likewise, undifferentiated pleomorphic sarcoma, angiosarcoma, and liposarcoma are some of the more common malignant (cancerous) soft tissue tumors. If the tumor is malignant and typically responds well to chemotherapy or radiation, then these adjuvant (additional) therapies may be utilized during the course of treatment. Pre-operative or postoperative radiation is often combined with surgical removal. The radiation gets rid of any microscopic cells that may re-grow and reduces the risk of the tumor coming back or recurring. Some soft tissue masses may be more difficult to remove than others depending on anatomical location, size, and involvement with surrounding major arteries, veins, or nerves. However, approximately 95% of soft tissue tumors can be removed while preserving the affected limb. In some instances the extremity cannot be saved and an amputation is performed. Contraindications for saving the limb may include neurovascular invasion, infection, pathological fracture, extensive disease, contamination from a poorly performed biopsy, recurrent disease.
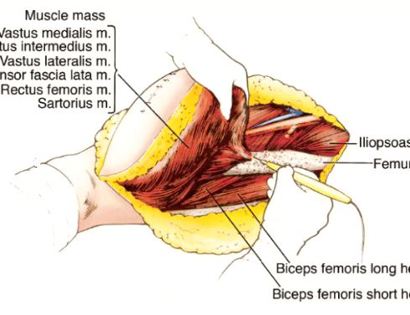
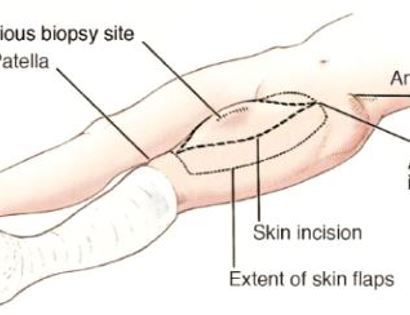
An incision is made surrounding the previous biopsy site to ensure that the tumor is properly removed.
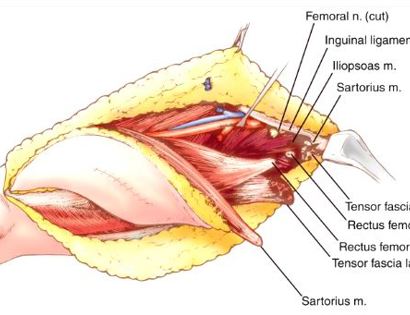
Developing surgical planes (margins that are tumor free) and separating muscles that can be preserved and leaving those in continuity with the tumor that should be removed. This is based on preoperative MRI and intraoperative findings as well as the type of tumor.
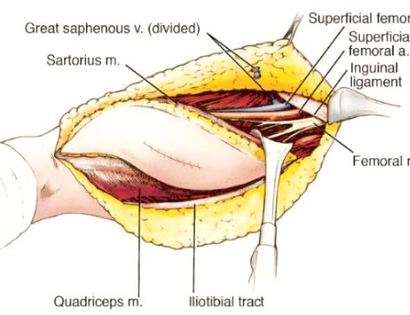
Separating important nerves and blood vessels from the sarcoma to preserve the important nerve and blood supply to the arm or leg. Sarcomas usually compress, displace and stretch these structures and rarely encase them. Once these are separated they are retracted gently and preserved throughout the surgery. Rarely, nerves and blood vessels may be removed with the tumor and then restored with various techniques.
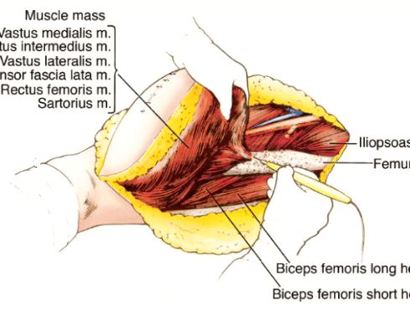
Remove the sarcoma en-bloc with a margin. Margins are also usually sent for analysis during surgery (frozen section analysis) to make sure there are no residual microscopic cells.
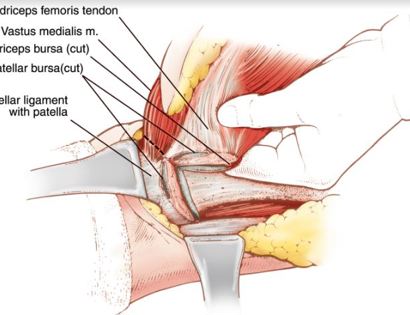
The tumor is typically removed with margins to ensure that the entirety of the tumor is resected from the patient.
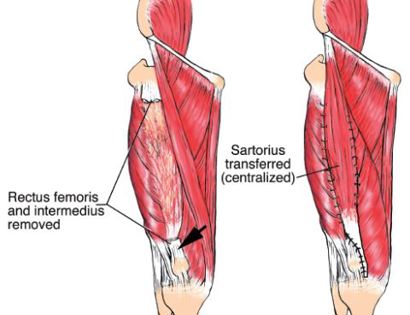
Reconstruction of the dead space is often accomplished with local muscle rotational flaps. This also may help restore function from the deficiency caused by removal. Occasionally a free microvascular free muscle flap may be performed where the muscle or tissue is harvested from a different area of the body with its attached blood vessels and moved to the defect and the vessels reattached to restore the blood supply to the muscle or tissues. The surgical bed is marked with hemoclips (small clips for blood vessels) so the area can be identified if radiation is needed after surgery.
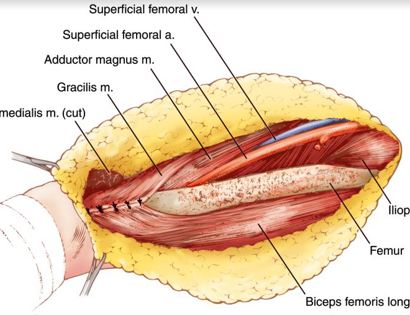
To reconstruct the area after the tumor is removed, muscle is attached and may be reinforced with surgical tape.
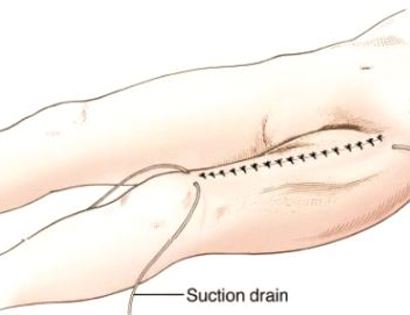
Closure and drains often placed for a period of time to evacuate fluid that can collect after surgery. Drains may be left in place for up to several weeks depending on size of defect, weight of patient and other factors until the wound heals. A bulky or compression bandage may be applied to control swelling and protect the extremity.
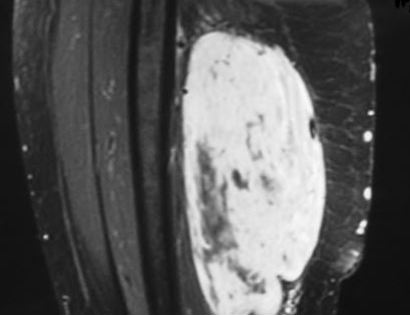
This is an example of a massive soft tissue tumor located in the back of the thigh.
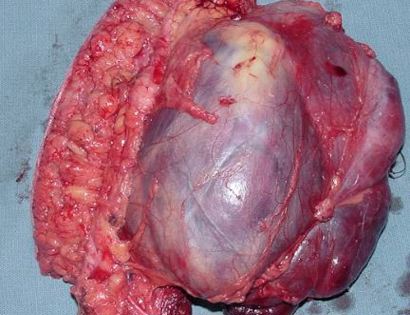
This is what the soft tissue tumor looked like after being removed from the patient.
After your surgery you may spend a few nights in the hospital depending on the type of surgery. Once discharged from the hospital, you will be recuperating at home. Various pain protocols and nerve blocks may be used to minimize pain. Mostly all patients are very comfortable after the surgery. For the first few days you will ice the area and keep it elevated to reduce swelling. Dr. Wittig usually wants you to keep the same bandages in place that were put on in the OR in a sterile manner and keep the site dry until you return to the office. You will usually return to the office 2 weeks after surgery. Once cleared, you will subsequently start physical therapy. We usually prescribe specific physical therapy protocols 3 times a week for 12 weeks after surgery to gradually strengthen muscles. Strengthening commences with significant resistance after sufficient range of motion is achieved as determined by Dr. Wittig. There may be an ultimate weight limit imposed upon you depending on various factors.
You will be monitored periodically with MRI imaging over the course of 5 years to ensure there are no signs of recurrence. You will also likely be monitored for metastases with a CT scan of the chest, abdomen and pelvis. You may, depending on size and grade of the sarcoma, have follow up appointments every 4 months for the first 2 years, then every 6 months for the next 2 years, and then once a year often up to year 10. For the best results, physical therapy protocols should be followed strictly. After radiation and a large surgery, some degree of swelling can be anticipated that could last a lifetime. A proper diet and weight control are imperative to optimize recovery and the ultimate functional result.
Dr. James Wittig narrates a video illustrating the surgical technique for resection of a soft tissue sarcoma. | WATCH VIDEO