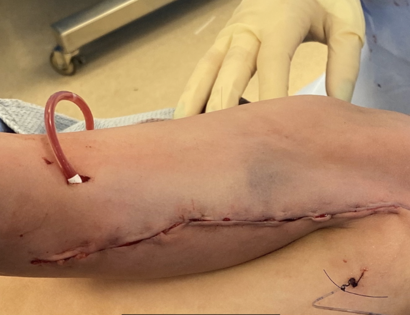
What is Limb Sparing Surgery of the Upper Arm/Shoulder?
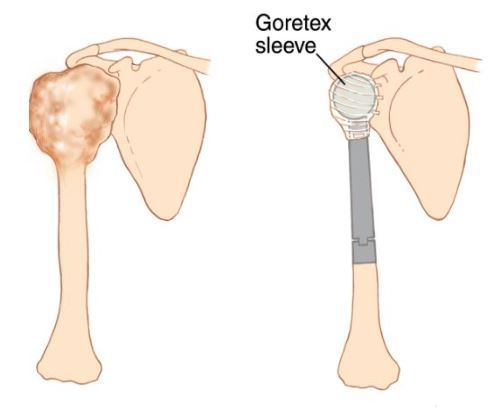
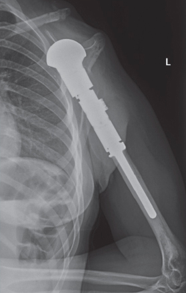
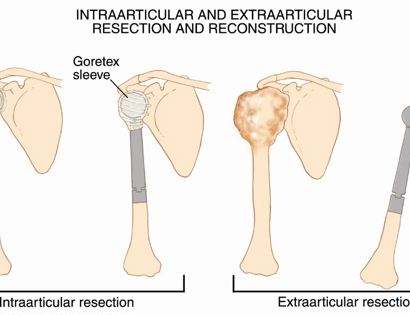
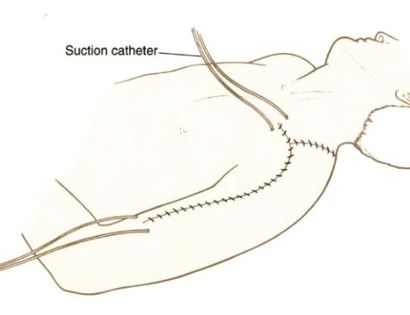
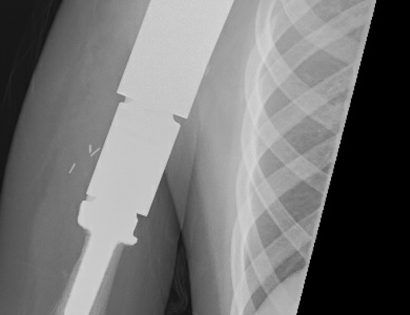
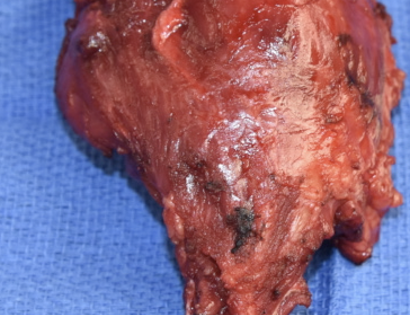
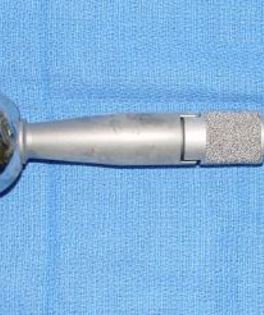
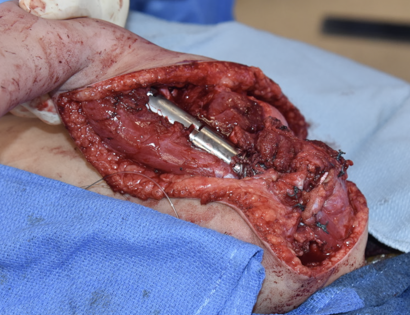
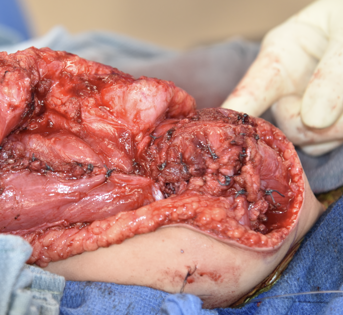
This is a procedure that involves removing a tumor of the upper arm bone, called the humerus. In most instances, the bone and shoulder are replaced with a special customizable prosthesis.
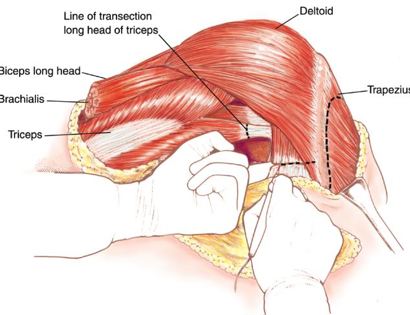
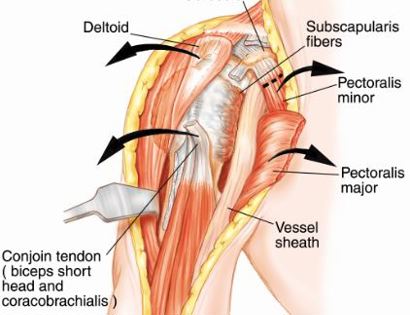
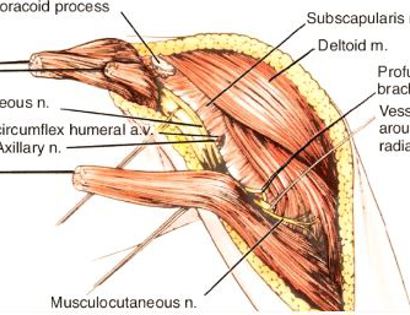
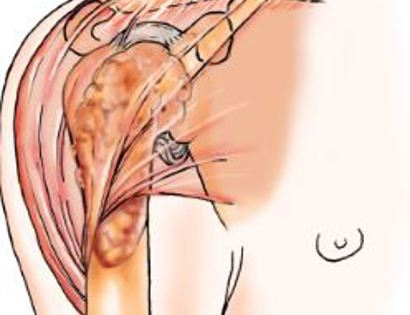
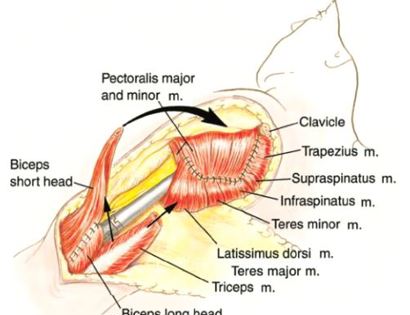
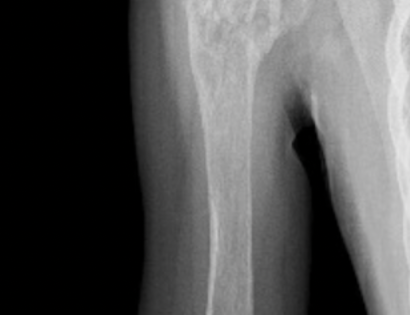
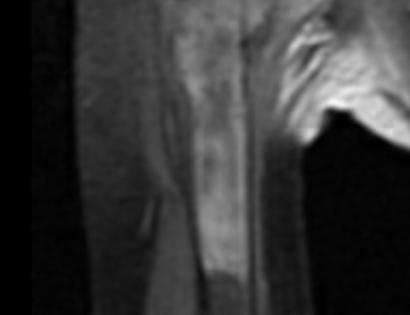
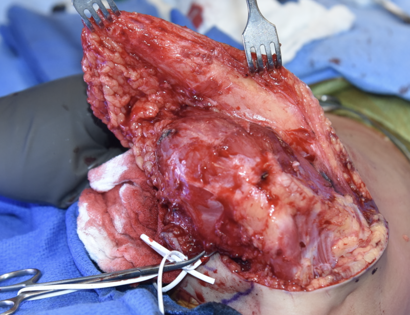
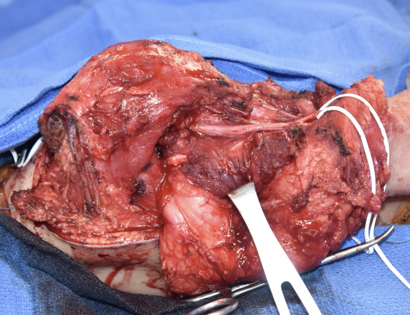
The shoulder girdle consists of the proximal humerus, scapula, and clavicle. Common tumors that affect the upper humerus are various sarcomas, benign aggressive tumors, and metastatic cancers to bone. Some of these tumors include osteosarcomas, chondrosarcomas, and giant cell tumors. Limb-sparing surgery can be performed for approximately 95% of tumors arising from the upper humerus. In some instances the extremity cannot be saved, and an amputation is performed.
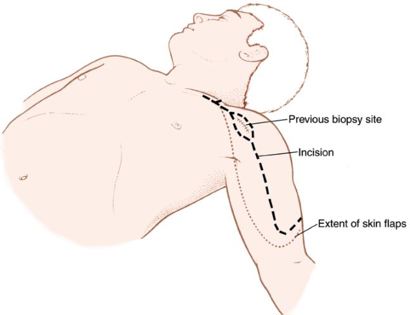
Contraindications for saving the limb may include neurovascular invasion, infection, pathological fracture, invasion of the chest wall, extensive disease, contamination from a poorly performed biopsy, recurrent disease.