Excision of Schwannomas
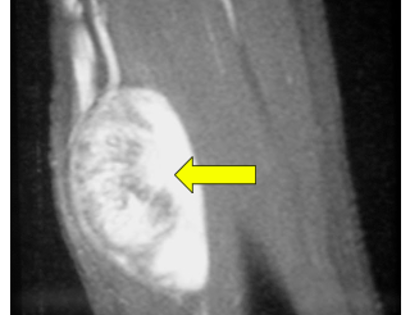
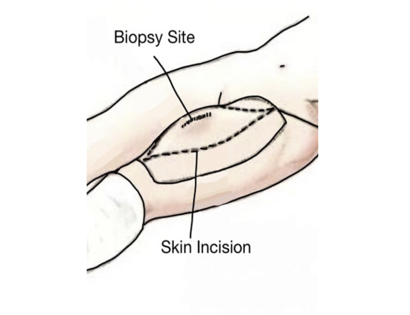
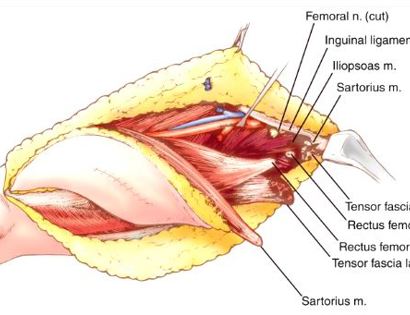
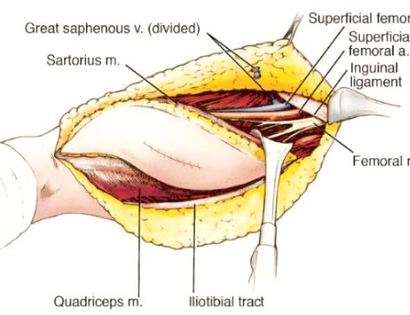
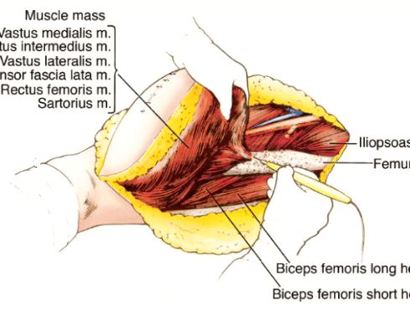
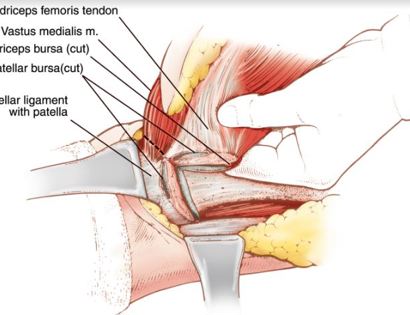
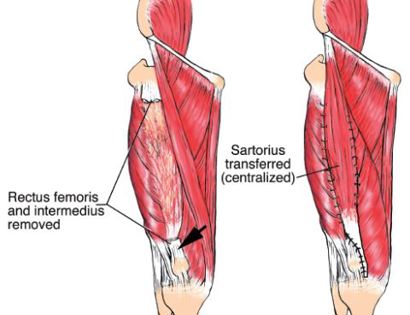
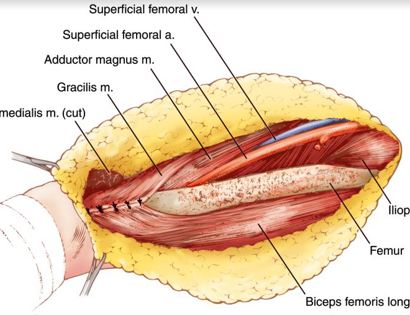
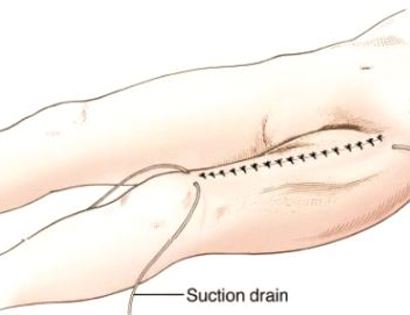
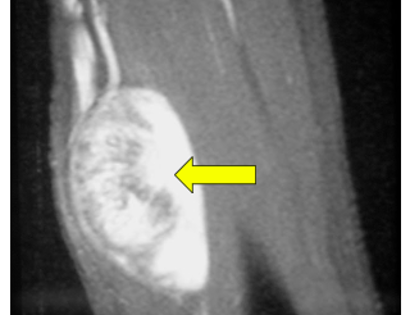
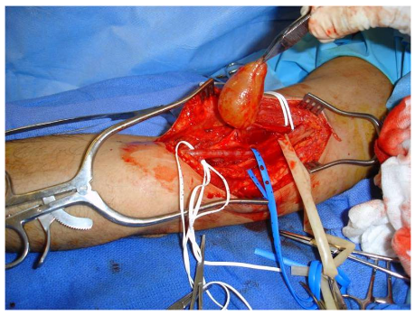
A schwannoma is a benign (non-cancerous), soft-tissue mass that presents on the outer, protective layer of a nerve, called the epineurium. To treat, a schwannoma can be marginally excised, meaning only the schwannoma is surgically removed, to spare or protect the nerve from excision.