Endoprosthetic Reconstruction
It is a procedure that involves removing a tumor (usually malignant or benign aggressive) of the bone and replacing it with a metal prosthesis to preserve the limb.
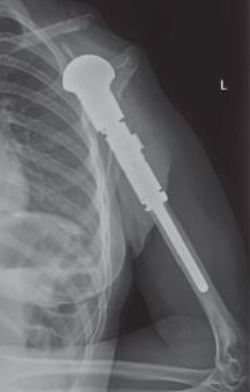
It is a procedure that involves removing a tumor (usually malignant or benign aggressive) of the bone and replacing it with a metal prosthesis to preserve the limb.

Limb salvage or limb sparing surgery refers to surgically removing a tumor of an extremity without performing an amputation. The limb is saved. In the past, most sarcomas were treated with an amputation. The most common sarcomas include osteosarcoma, ewing’s sarcoma, and chondrosarcoma. They will predominantly arise in the femur (thigh bone) humerus (long bone of arm), tibia (shinbone), and scapula. Reconstruction of the limb to avoid amputation has become an exciting and groundbreaking moment in the field to restore function and quality of life. Endoprosthetic reconstruction is the surgical procedure performed instead of an amputation and utilizes a metal prosthesis to provide a functional limb. Today, approximately 95% of patients can be treated with a limb sparing surgery instead of an amputation.

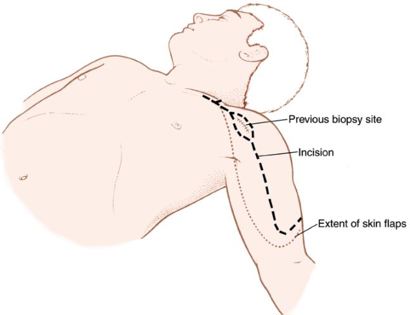
The previous biopsy sit is marked and the incision is made leaving a decent margin so that there is no tumor remaining after it is removed.
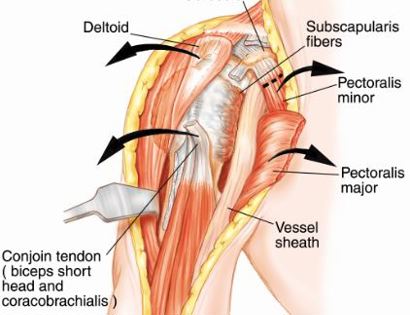
Developing surgical planes (margins that are tumor free) and separating muscles that can be preserved and leaving those in continuity with the tumor that should be removed. This is based on preoperative MRI and intraoperative findings as well as the type of tumor.
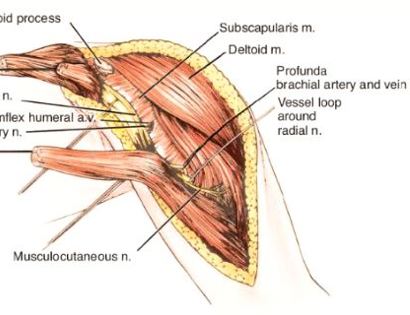
The first step in the removal of bone tumors is removing the lesion with a margin of normal bone and soft tissue around it. During the removal portion of the procedure, all major arteries, veins, and nerves are identified and separated from the tumor. In rare cases a nerve (s) may need to be removed if it is involved by the tumor. The location and size of the bone tumor will determine which major vessels (veins and arteries) and nerves need to be mobilized away from the tumor so that it can safely be resected.
Removal of tumor and reconstruction. Once the tumor is removed, reconstruction of the limb is performed utilizing a customizable tumor prosthesis. This prosthesis is sized and built during the surgical procedure then implanted with cement to secure it in place, or sutured to surrounding muscles. In some instances for pediatric patients, the prosthesis used has a unique ability to extend for patients that are not skeletally mature (growth plate has not closed yet). This ultimately prevents any leg length discrepancy so quality of life is not compromised. The patients will come in for office visits and an MRI like machine will use a “rotating mechanism” over the patients prosthesis to enable it to rotate and extend. This is a non-invasive and pain free intervention for these pediatric patients.
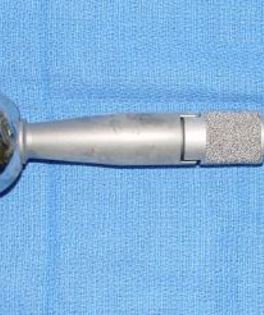
This prosthesis is sized and built during the surgical procedure then implanted. We cement the prosthesis into your bone and safely secure it in place.
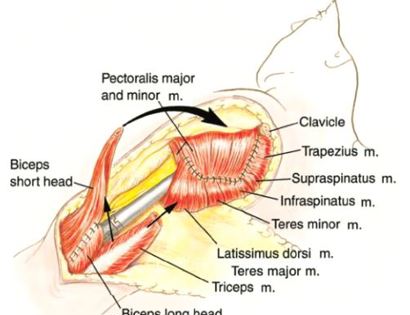
Once the tumor prosthesis has been successfully implanted, surrounding muscles may be utilized to reconstruct the area and provide soft tissue coverage of the prosthesis. The soft tissue coverage utilizing your muscles not only provides additional support to your prosthesis, but also helps prevent skin problems and infections after your surgery.
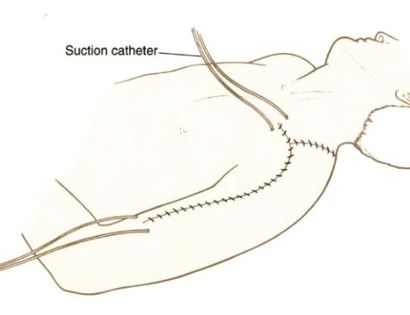
We then perform closure your incision with sutures and cover the surgical site with bandages. Multiple large drains may also be used to drain the surgical site and prevent a seroma (build up of fluid).
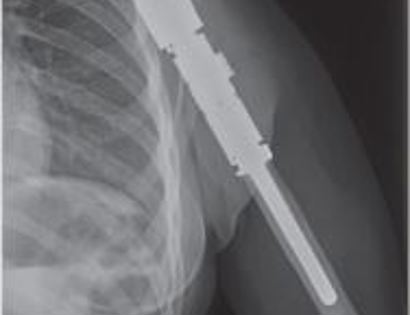
This is an x-ray image of an endoprosthesis in the arm. The prosthesis is made to match the length of the original bone and soft tissue reconstruction covers the prosthesis to maximize functioning postoperatively.
After your surgery you may spend a few nights in the hospital depending on the type of procedure. Once discharged from the hospital, you will be recuperating at home. Various pain protocols and nerve blocks may be used to minimize pain. Mostly all patients are very comfortable after the surgery. For the first few days you will ice the area and keep it elevated to reduce swelling. Dr. Wittig usually wants you to keep the same bandages in place that were put on in the OR in a sterile manner and keep the site dry until you return to the office. You will usually return to the office 2 weeks after surgery. Once cleared, you will subsequently start physical therapy. We usually prescribe specific physical therapy protocols 3 times a week for 12 weeks after surgery to gradually strengthen muscles. Strengthening commences with significant resistance after sufficient range of motion is achieved as determined by Dr. Wittig. There may be an ultimate weight limit imposed upon you depending on various factors.
You will be monitored periodically with MRI and X-ray imaging over the course of 5 years to ensure there are no signs of recurrence. You will also likely be monitored for metastases with a CT scan of the chest, abdomen and pelvis. You may, depending on size and grade of the sarcoma, have follow up appointments every 4 months for the first 2 years, then every 6 months for the next 2 years, and then once a year often up to year 10. For the best results, physical therapy protocols should be followed strictly. After radiation and a large surgery, some degree of swelling can be anticipated that could last a lifetime. A proper diet and weight control are imperative to optimize recovery and the ultimate functional result.
Dr. James Wittig narrates a video illustrating the surgical technique for an endoprosthetic reconstruction procedure. | WATCH VIDEO