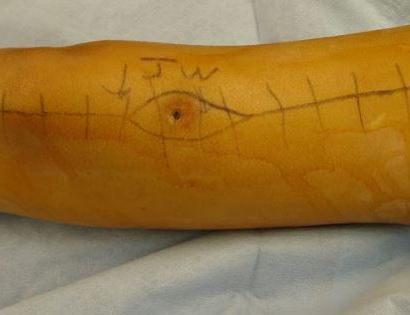
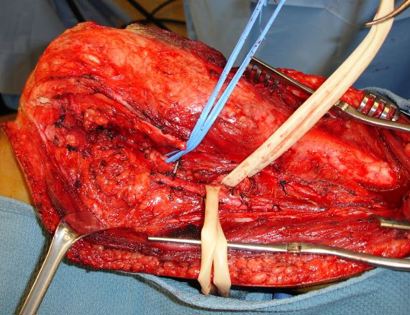
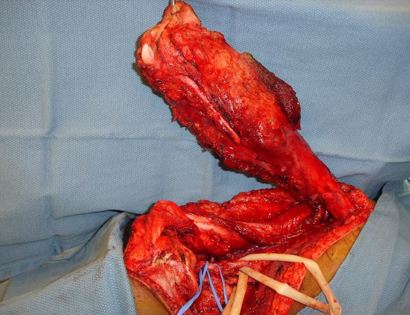
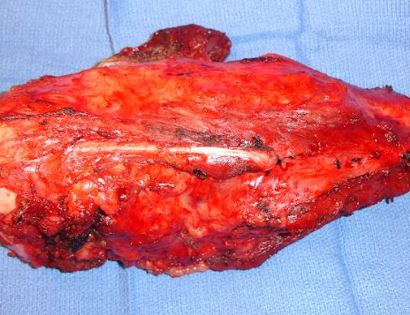
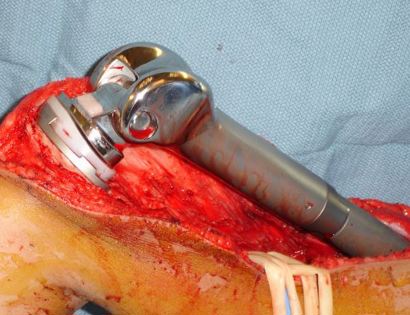
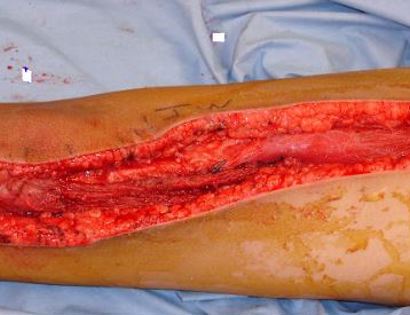
What is a Limb-Sparing Surgery of the Lower Leg/Knee?
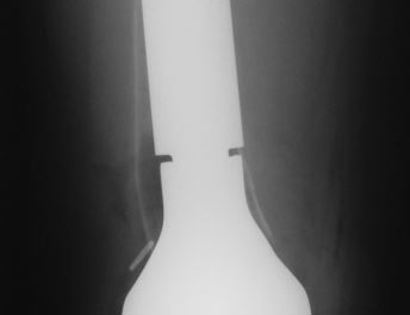
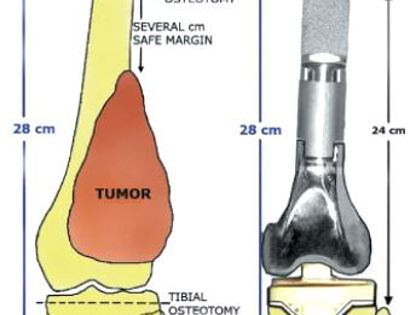
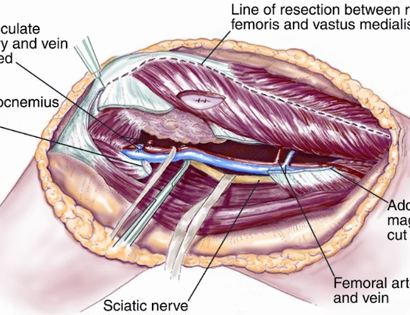
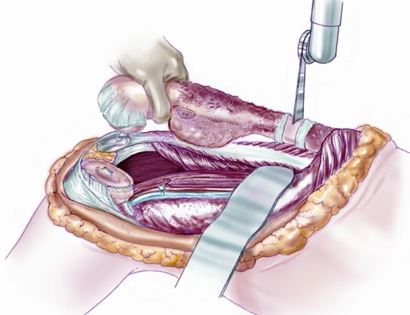
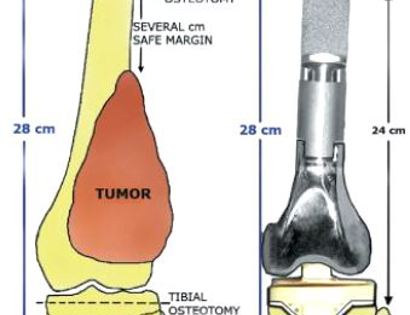
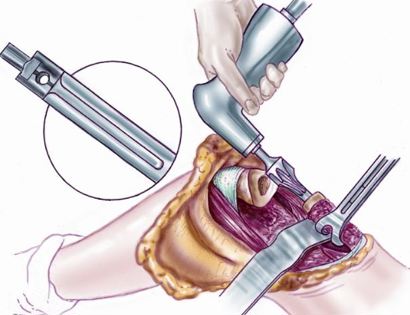
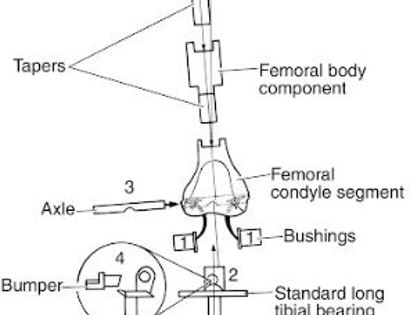
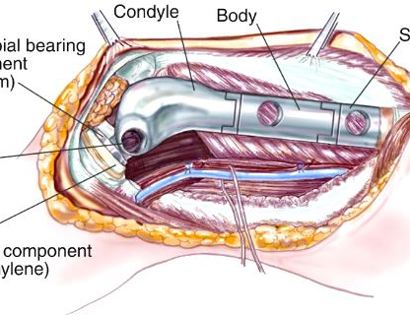
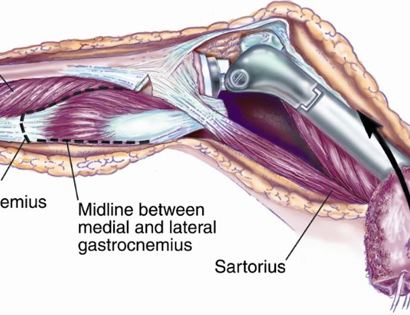
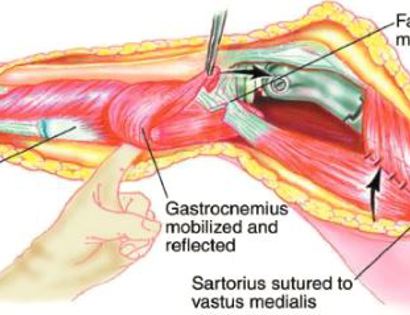
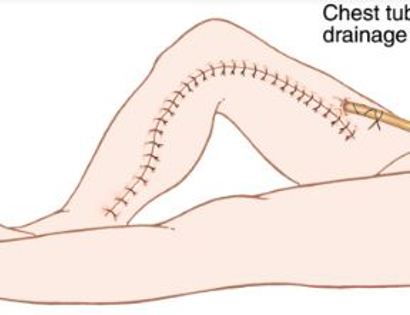
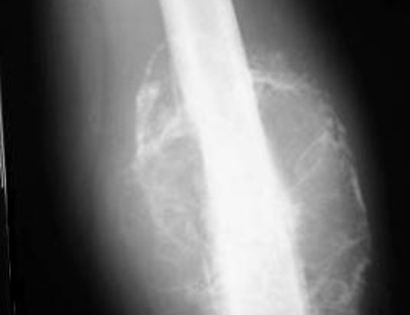
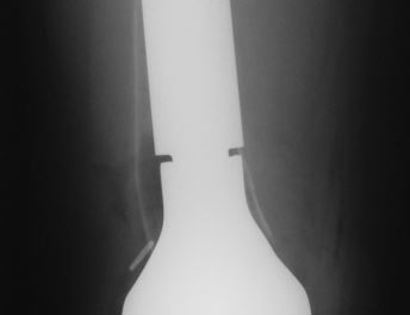
The knee joint consists of your femur, tibia, fibula, and patella. The distal (lower portion) femur and its diaphysis (middle portion) are common sites for primary bone sarcomas and metastatic tumors. Some of these tumors include osteosarcomas, chondrosarcomas, and ewing’s sarcomas. Limb-sparing surgery can be performed for approximately 95% of tumors arising from the lower femur. In some instances, the extremity cannot be saved and an amputation is performed.
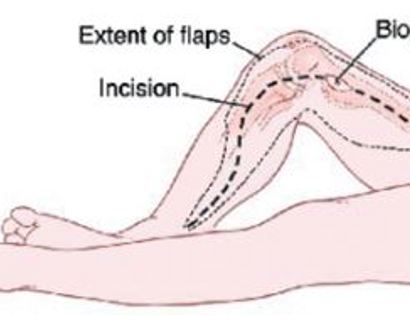
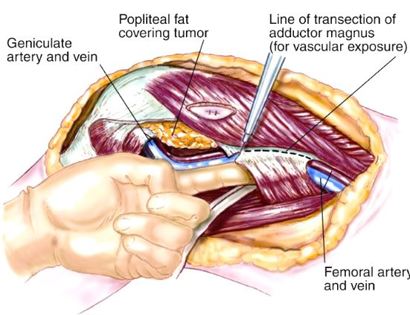
Contraindications for saving the limb may include neurovascular invasion, infection, pathological fracture, extensive disease, contamination from a poorly performed biopsy, recurrent disease.