Dedifferentiated Liposarcoma
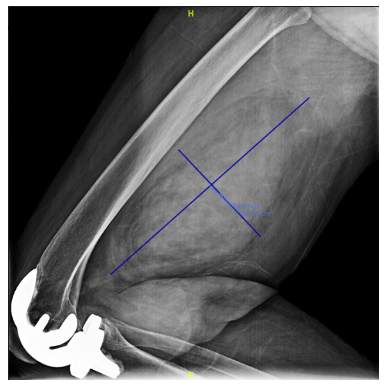
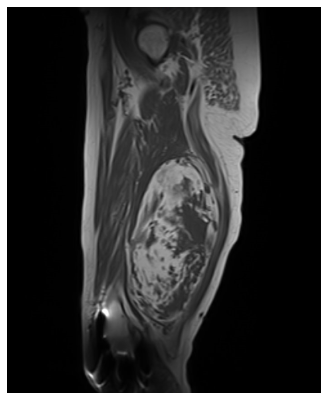
Dedifferentiated Liposarcoma is a malignant (cancerous), soft-tissue sarcoma that most commonly occurs in the retroperitoneum, or the area in the back of the abdomen. It is an atypical liposarcoma that can arise from a low-grade, well-differentiated liposarcoma that can progress overtime into a dedifferentiated liposarcoma. Treatment includes surgical resection or removal of the tumor.